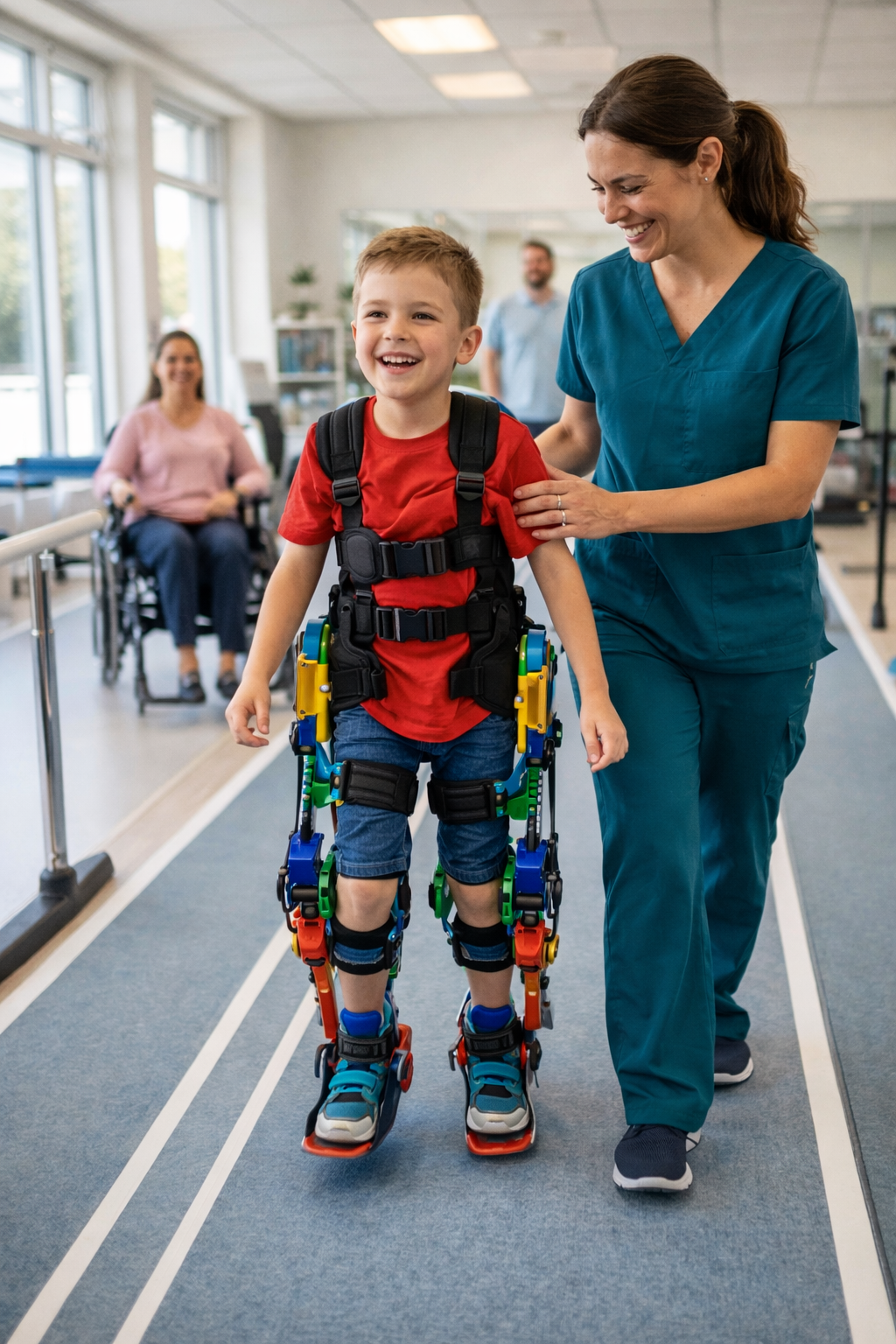
Imagine a world where a child, once limited in their ability to stand or walk independently, can rise from a wheelchair and move through their environment, participating more fully in life’s activities. This is the promise and the emerging reality of pediatric exoskeletons—advanced robotic devices designed specifically for children with mobility impairments. These remarkable technologies are not just high-tech gadgets; they are powerful tools with the potential to fundamentally transform traditional physical and occupational therapy and, crucially, a child’s real-world functional abilities. This article will explore what pediatric exoskeletons are, the various types and their conditions they support, the profound ways they are reshaping rehabilitation, and the practical landscape of accessing them today.
Key Takeaways
- Pediatric exoskeletons are wearable robotic devices that assist or augment a child’s movement, primarily focus on gait and upper limb function.
- They provide consistent, intensive, and repeatable training that is difficult to achieve with manual therapy alone.
- The real-world transformation extends beyond physical metrics to cognitive, social, and psychological benefits, fostering greater independence and confidence.
- Current challenges include high cost, limited insurance coverage, the need for specialised therapist training, and ongoing technical refinements.
- The future is optimistic, with advancements promising lighter, more intelligent, and more accessible devices that integrate more seamlessly into a child’s daily life.
Who This Is For
This comprehensive guide is designed for parents and caregivers of children with mobility impairments seeking information about innovative rehabilitation options. It is also a valuable resource for pediatric physical and occupational therapists, healthcare providers, and anyone interested in the intersection of robotics, assistive technology, and child development.
Safety Disclaimer: It is essential to understand that pediatric exoskeletons are medical devices and must be prescribed and used under the strict guidance and supervision of a trained physical therapist or healthcare professional. Improper use or fit can lead to injury. This information is for educational purposes and should not replace professional medical advice or a comprehensive evaluation to determine suitability for an individual child.
Understanding Pediatric Exoskeletons: More Than Just Robots
At their core, pediatric exoskeletons are wearable robotic systems designed to improve the physical capabilities of a child. But what does that really mean, and how do they function differently from other assistive technologies like walkers or traditional orthoses? Let’s delve into the mechanics and classifications.
Technology and Mechanics
Pediatric exoskeletons combine sophisticated engineering with an understanding of human biology. While specific designs vary, most consist of a rigid or semi-rigid external structure that aligns with the child’s body. Integrated sensors monitor the child’s movements and intentions. These sensors feed data into powerful onboard computers running complex control algorithms.
Based on this information, high-performance motors or actuators provide the precise level of force or assistance needed at specific joints (like hips, knees, and ankles) to facilitate a natural movement pattern. Some devices can provide 100% of the movement power, while others are designed to dynamically assist and adapt as the child grows stronger. For children with significant weakness, the exoskeleton provides the structure and power they lack, enabling movement that would otherwise be impossible. For those with some motor function, the device can provide assistance only when needed, encouraging active user participation.
Types and Functions
To best meet the diverse needs of children, various types of exoskeletons have been developed and are continually being refined. They can be broadly classified based on:
1. Body Part Assisted: Lower Limb vs. Upper Limb
- Lower Limb Exoskeletons: These are currently the most common type, focusing on walking, standing, and gait training. They range from large, clinic-based systems to smaller, more portable devices for potential real-world use. They help address issues like drop foot, crouching gait, and poor symmetry in children with cerebral palsy, spinal cord injuries, or muscle diseases.
- Upper Limb Exoskeletons: These assist with reaching, grasping, and manipulating objects. They can target specific joints like the elbow, wrist, or individual fingers, or support the entire arm. While less prevalent than lower-limb options in pediatric settings, upper limb exoskeletons are crucial for improving independent daily activities like eating, dressing, and playing for children with conditions affecting hand and arm function.
2. Mode of Actuation: Active vs. Passive vs. Hybrid
- Active Exoskeletons (Powered):: These are equipped with motors and an internal power source (like a battery pack). They can provide full or partial assistance, actively driving movement for the user. They are best for children with severe motor impairments.
- Passive Exoskeletons: These devices don’t have motors. Instead, they use materials like springs, tension bands, or pneumatic systems to store and release energy, correct posture, or offset the weight of a limb, making movement easier. They are often lighter and less complex but offer limited assistance.
- Hybrid Exoskeletons: A combination approach, using passive elements for some functions and active motors for others, aiming for an optimal balance of assistance, weight, and complexity.
The Power of Real-World Transformation: From Therapy to Daily Life
The true measure of any rehabilitation tool is its impact on a person’s ability to participate in and enjoy life outside the clinical setting. This is precisely where pediatric exoskeletons are demonstrating their unique value. They provide a level of intensive, repeatable, and task-specific training that is challenging, if not impossible, to achieve through manual therapy alone.
Intensive and Goal-Directed Practice
Neuroplasticity, the brain’s ability to reorganize itself by forming new neural connections, is a fundamental principle of rehabilitation, especially in children whose nervous systems are still developing. Successful neurorehabilitation requires repetitive, intensive, and correct practice of specific movements.
In traditional child gait training, a physical therapist manually guides a child’s limbs, which is physically exhausting for the therapist and can be limited in duration and consistency. Exoskeletons can perform thousands of steps with precise accuracy, ensuring each movement reinforces the correct neural pathways. The device can collect real-time data on the child’s effort, gait pattern, and progress, allowing for highly personalised and progressively challenging therapy sessions that directly target functional goals, like walking to the bathroom, playing catch, or navigating school hallways.
Real-World Benefits and Practical Examples
The benefits go far beyond walking metrics. Let’s look at illustrative examples:
- A child who once required significant manual assistance to walk across a room can now, with the help of a lower-limb exoskeleton, independently navigate a playground or go for a walk in the park. This improves endurance and physical health while offering newfound freedom.
- A child with upper-limb weakness can now use an exoskeleton to feed themselves independently, drawing a sense of accomplishment and dignity in a core life activity.
- The improved upright posture and consistent gait provided by a lower-limb device can lead to better digestion, bladder control, and reduced risk of contractures and joint deformities that are common issues for children with significant mobility challenges. This has long-term positive health implications.
- The ability to interact with peers while standing or walking at eye level can profoundly affect a child’s social and psychological well-being, fostering greater participation and confidence.
Dynamic Orthoses vs. Exoskeletons: A Vital Distinction
It’s crucial to understand the difference. Traditional dynamic orthoses (like AFOs or KAFOs) are passive devices that primarily provide static support, alignment, and prevent deformity. They do not add power to the child’s movements. In contrast, most effective pediatric exoskeletons are active devices that provide powered assistance and are explicitly designed as robotic rehabilitation tools for training and functional improvement, not just static support. They are closer to dynamic therapy partners than traditional braces.
Practicalities and Challenges in the Real World
While the potential is incredible, it’s vital to have a realistic understanding of the current real-world landscape for pediatric exoskeletons.
Cost and Accessibility: Navigating the Hurdles (As of July 2024)
This is one of the most significant practical challenges. Pediatric exoskeletons are sophisticated medical devices with high development and manufacturing costs. Generally, a single device can cost upwards of a significant amount, which is beyond the means of most families.
Currently (As of July 2024), insurance coverage in many regions, including the United States, is extremely limited and inconsistent. Most devices are not yet classified for broad and automatic coverage. Families often face a complex, multi-year process involving numerous medical evaluations, letters of medical necessity from a dedicated clinical team, and a series of prior authorization requests and potential appeals. Some device manufacturers offer assistance programs, but they are limited. Clinical research and development are ongoing to reduce manufacturing costs, build a stronger evidence base for efficacy, and ultimately, advocate for broader insurance coverage.
The Vital Role of Therapists and Families
An exoskeleton is a tool, not a standalone solution. A trained physical therapist is essential for:
- Initial evaluation and patient selection: Not all children are suitable candidates.
- Customized fitting and programming: Tailoring the device settings to the child’s changing needs and growth.
- Conducting intensive and goal-directed training sessions.
- Ongoing progress assessment and readjustment.
Families play a critical role, not only in navigating the logistical and financial process but also in supporting the intensive therapy commitment, providing encouragement, and learning how to integrate the device (if portable) safely and effectively into the child’s daily life. Proper training for both therapists and families is non-negotiable for safe and successful use.
Safety Considerations and Limitations
Pediatric exoskeletons have specific weight and height ranges. They are not suitable for children with severe joint contractures, certain bone conditions, uncontrolled seizures, or significant skin issues. Proper fitting is paramount to prevent pressure sores or other injuries. Battery life, device weight, and potential for technical glitches are other practical considerations.
Common Mistakes and Misconceptions
There are several prevalent misconceptions that can create unrealistic expectations or hinder the effective use of pediatric exoskeletons. Here are a few to avoid:
- Exoskeletons Are a “Cure” for Mobility Impairments: Absolutely false. These are tools to manage symptoms, improve function, and support independence. They do not reverse underlying conditions. Thinking of them as a magical fix can lead to profound disappointment and may cause families to de-prioritize other essential aspects of care, such as speech therapy or education.
- They Replace Therapists: This is a massive mistake. Exoskeletons are a force multiplier for a skilled therapist. Without the expert guidance of a trained professional, the device cannot be used to its full potential, and improper use can even be unsafe. The goal is collaborative, human-led, and tech-supported neurorehabilitation.
- Any Child Can Benefit: As discussed in the safety section, patient selection is crucial. Factors like weight, height, bone density, and specific impairments must be carefully considered. It’s vital to get a thorough professional evaluation.
- They Are a “Set It and Forget It” Device: In reality, using an exoskeleton requires careful, expert setup and constant monitoring. A child will need ongoing assessments, programming updates as their abilities change, and potential modifications as they grow.
- All Exoskeletons Are the Same: The differences between types (lower- vs. upper-limb, active vs. passive) and brands are significant. Do thorough research and consult with your medical team to find the best fit for your specific child’s needs.
Conclusion
The emergence of pediatric exoskeletons represents a true paradigm shift in the world of rehabilitation for children with mobility impairments. They offer new ways to address old challenges, moving beyond traditional therapy limitations to enable consistent, intensive, and goal-directed training. More than that, they provide a powerful new path towards improved function, greater social integration, and improved self-confidence for children who face significant physical hurdles.
However, the real-world transformation is not instantaneous, nor is it without significant practical challenges. High costs, complex insurance processes, and technical and safety considerations are hurdles that require careful navigation and ongoing advocacy. Yet, the rapid pace of technological advancement and the growing body of supportive clinical research provide a foundation for optimism.
If you are a parent, caregiver, or professional in this field, the most important next steps are:
- Research: Familiarize yourself with the current technology and types of devices.
- Consultation: Seek out specialized pediatric rehabilitation centers that have experience with these technologies. Discuss with your child’s pediatrician, orthopedist, and physical therapist whether an exoskeleton evaluation is appropriate.
- Advocacy: Stay informed and support efforts to increase research funding, reduce manufacturing costs, and improve insurance access.
The journey may be challenging, but for many children and families, the transforming potential of pediatric exoskeletons in the real world is a beacon of hope and a powerful tool for unlocking a child’s true potential for a fuller, more independent life.
Frequently Asked Questions
What are pediatric exoskeletons and how do they work? Pediatric exoskeletons are wearable robotic devices that assist or augment movement in children with mobility impairments. They typically use a combination of sensors, an onboard computer, control algorithms, and motors (in active devices) to provide precise assistance at specific joints to facilitate a more natural walking or movement pattern.
Which children can benefit from these devices? Exoskeletons can potentially benefit children with a range of conditions affecting mobility, including cerebral palsy, spinal cord injuries, certain forms of muscular dystrophy, spina bifida, and acquired brain injuries. However, patient selection is crucial and based on factors like condition severity, age, weight, and other medical considerations.
Are they considered a “cure” for mobility impairments? No, exoskeletons are not a cure. They are advanced therapeutic and assistive tools designed to improve functional mobility, increase independence, and reduce the risk of secondary health complications. They do not reverse the underlying medical condition.
How much do they typically cost and does insurance cover them? (As of July 2024) Cost is a major hurdle, with devices generally costing a significant amount. Insurance coverage as of July 2024 is extremely limited and inconsistent, with many families requiring significant time and advocacy to secure coverage or alternative funding.
What are the typical therapy requirements when using an exoskeleton? Exoskeletons are typically used as part of an intensive, goal-directed physical therapy program. This involves regular, long-term sessions, expert guidance from a trained physical therapist, and significant commitment and involvement from families. They are a tool for, not a replacement of, manual therapy.
Are there specific age or weight limitations for children? Yes, each device has specific manufacturer-recommended height, weight, and age ranges. Thorough professional evaluation is always required. Exoskeletons are not suitable for all children with mobility issues.
References
- Source: American Physical Therapy Association (APTA) – Private Practice Section Blog. Type: Organization Publication. Description: Provides insights into innovative pediatric physical therapy approaches, highlighting the human element alongside emerging tech. Search: ‘Getting Kids Moving: Pediatric Physical Therapy | APTA Private Practice’
- Source: National Institutes of Health (NIH) Clinical Center News. Type: Official Government News Release. Description: Detailed article on an early pediatric exoskeleton clinical study and its potential. Search: ‘Robotic exoskeleton offers potential new approach to alleviating crouch gait NIH’
- Source: Journal of NeuroEngineering and Rehabilitation (JNER). Type: Peer-Reviewed Academic Journal. Description: Source for scholarly research papers on neurorehabilitation and robotic assistive devices. Search: ‘Pediatric exoskeleton gait training children cerebral palsy spina bifida research JNER’
- Source: Brooks Rehabilitation. Type: Independent Rehabilitation Hospital System. Description: Provides information on their clinical use of advanced technologies like exoskeletons. Search: ‘Lower-Limb Therapy with the Indego Exoskeleton | Brooks Rehab’
- Source: American Academy for Cerebral Palsy and Developmental Medicine (AACPDM). Type: Professional Medical Academy. Description: A primary source for clinical guidelines, research summaries, and education related to cerebral palsy. Search: ‘AACPDM robotic rehabilitation technology for children with cerebral palsy’
- Source: International Society of Physical and Rehabilitation Medicine (ISPRM). Type: International Professional Medical Society. Description: Global organization promoting physical and rehabilitation medicine. Search: ‘ISPRM pediatric rehabilitation technology robotics advancements’
- Source: National Spinal Cord Injury Association. Type: Patient Advocacy Organization. Description: Resources and support for individuals with spinal cord injuries, including info on assistive tech. Search: ‘Spinal Cord Injury Association pediatric assistive devices mobility solutions’
- Source: Cerebral Palsy Foundation. Type: Patient Advocacy Organization. Description: Focuses on research, advocacy, and quality of life for individuals with CP. Search: ‘Cerebral Palsy Foundation emerging therapies technology pediatric care’